Overview | Understanding the Disorder | Symptoms | Diagnosis |
Treatment | Frontiers
Vocal Fold Scar:
Abnormal scar tissue in the vibrating layer of the vocal fold that causes voice problems
Lamina Propria:
Vibrating component of the vocal folds that covers the vocal fold muscle or body; the lamina propria is composed of three layers: superficial, intermediate, and deep lamina propria
Mucosal Wave:
Wave-like motion of the vibrating layer of the vocal fold as seen upon slow motion-like viewing through stroboscopy
Stroboscopy:
Laryngoscopy with synchronized strobe light that provides a slow motion-like view of vocal fold vibration (mucosal wave); stroboscopy is the key tool used to analyze vocal fold vibration
How is vocal fold scar diagnosed?
An otolaryngologist can make a diagnosis of vocal fold scar from a patient history and a laryngeal examination. If vocal fold scar is suspected after a review of the patient’s voice symptoms, the otolaryngologist will examine the voice and voice box to confirm diagnosis.
Voice Quality Assessment
Patients with vocal fold scar will typically have a roughness, breathiness or weakness to the voice. Often, a strained sound is associated with vocal fold scar.
The physician will also note whether a patient is attempting to compensate for or adapt to vocal fold scarring by speaking in an unnaturally low pitch or high pitch (“compensated falsetto”).
Stroboscopy is Key Diagnostic Test
The most important method in vocal fold scarring diagnosis is stroboscopy. Stroboscopy allows the examiner to observe vocal fold vibration in “slow motion” during voice production. From this examination and observation, the nature of the vocal fold vibration, specifically the mucosal wave, can be observed. (For more information, see Laryngoscopy/Stroboscopy.)
Abnormal Mucosal Wave
Stroboscopy reveals the movement of the vibrating layer that occurs during vocal fold vibration. Strobosocopy combines laryngoscopy with synchronized rapid light pulses, thus providing a slow-motion-like view of vocal fold vibration.
- In reality, vocal fold vibration is extremely fast. Stroboscopy is necessary to create a slow-motion-like, simulated view of vocal fold vibration. This view is referred to as the “mucosal wave”. (Note: the vocal folds are not really “slowed down”; rather, the strobe light provides a simulated slow-motion-like picture of the different phases of the vibratory cycle.) (For more information, see Anatomy and Physiology of Voice Production.)
- The mucosal wave is changed when vocal fold scar is present. Normally, the mucosal wave is rapid and regular and with good reach in its movement (amplitude). Vocal fold scar causes the mucosal wave to be irregular and/or reduced in both speed and extent of movement (amplitude).
Typical Findings in Vocal Fold Scar
Typical findings from stroboscopy in patients with vocal fold scar include:
- decrease in the extent of movement (amplitude) of the mucosal wave seen during vocal fold vibration
- abnormality of vocal fold closure during vocal fold vibration
- decreased or stiffened appearance of mucosal wave
- incomplete vocal fold closure or a shortened duration of closure
Incomplete vocal fold closure is an extremely important diagnostic finding because it directly indicates vocal fold scarring, and correlates with the breathiness and increased effort that is commonly experienced by patients with vocal fold scar.
How Vocal Fold Scar – No Matter How Small – Can Hamper the Vibratory Cycle
| Normal | ||
|---|---|---|
| 1 Column of air pressure moves upwards towards vocal folds in “closed” position2, 3 Column of air pressure opens bottom of vibrating layers |
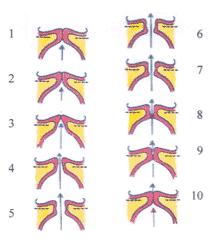 click for larger image click for larger image |
6-10 The low pressure created behind the fast-moving air column produces a “Bernoulli effect” which causes the bottom to close, followed by the top10 Closure of the vocal folds cuts off the air column and releases a pulse of air [ |
| Abnormal: Vocal Fold Scar – Impact on Opening and Closing during Vibratory Cycle | ||
| 2 Stiffness from “Scar |
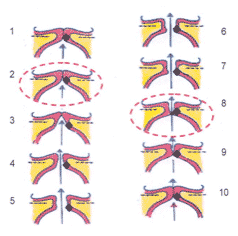 click for larger image |
8 Stiffness from “Scar |
Although quite simplified, this is a schematic representation of what could go wrong when one has scarred vocal folds.
Scarring affects the vibration of the vocal folds making it harder to open (panel 2) and harder to close (panel 8) compared to normal vocal folds (see normal vocal fold parallel diagram). Hence, patients with scarring in one or both vocal folds usually complain of increased effort and therefore voice fatigue. Depending on severity of scarring, the voice may be hoarse all the time, or just when added inflammation occurs as when one has a cold or reflux laryngitis. Also, when a cold goes away, the hoarseness that was precipitated by the cold does not go away when the cold lifts because the scarred area would be expected to heal slower if not worsen with each inflammatory insult.
Panel 2 also depicts the increased air pressure needed to open a scarred vocal fold and the asymmetry in vibration (cycles of opening-closing) when one fold is stiffer (the scarred vocal fold) than the normal vocal fold. This would be reflected in a change of voice quality that would be more noticeable on singing. Worse scar leads to worse voice changes.
- Scarring at the inferior (bottom) edge of the closing (striking) surface of the vocal folds is harder to detect. Usually the superior (top) edge of the closing surface can and will compensate.
- With increasing scar extent or severity, loss of vocal fold pliability increases, thus hampering additional phases of the vibratory cycle – and resulting in more severe voice symptoms.
Extent of Vocal Fold Scar
Focal vocal fold scar: Scarring that involves a small portion of one or two of the vocal folds
Full-length vocal fold scar: Scarring that extends the length of one or both of the vocal folds, depending upon the severity of the condition
Associated Lesions
Stroboscopy can also detect vocal fold lesions, such as cysts or polyps, that may or may not be associated with the presence of vocal fold scar. (For more information, see Vocal Fold Lesions.)
Key Role of Stroboscopy in Detection of Vocal Fold Scarring
Stroboscopy is necessary to assess vocal fold vibratory pattern (mucosal wave) during voice production. Abnormality in vocal fold vibratory pattern is a key indication that vocal fold scar is most likely present.
- Without stroboscopy, the diagnosis of vocal fold scarring can easily be missed.
Microlaryngoscopy Is a Powerful Diagnostic Adjunct
Microlaryngoscopy is another important diagnostic step that is sometimes required to fully assess the nature of the vocal fold scar – especially when other conditions such as vocal fold lesions make it difficult to assess the presence and extent of scarring.
- Microlaryngoscopy is performed with the patient under anesthesia. While the patient is asleep, the laryngologist uses a microscope to obtain a highly magnified view of the voice box – a better view than can be achieved by a mirror examination. Additionally, the surgeon can gently and thoroughly palpate the vocal folds, allowing an assessment of the size, nature, and location of the vocal fold scar.
- Microlaryngoscopy is also indicated when:
- Voice disorders cannot be completely explained by office examination techniques
- Patient cannot tolerate in-office examination techniques due to a strong gag reflex
Patient Informed Consent: Anesthesia Risk Versus Diagnostic/Treatment Gains
Microlaryngoscopy is performed routinely and without incident, however anesthesia is not without risk. Microlaryngoscopy should therefore be performed only when indicated, and patients should be informed regarding potential risks.
Vocal Fold Scar Can Cause Inadequate Closure of Vocal Folds
Often, incomplete vocal fold closure seen on stroboscopy is attributed to vocal fold muscle weakness (paresis). Poor vocal fold closure most likely indicates either vocal fold paresis or vocal fold scarring. (For more information, see Vocal Fold Paresis/Paralysis.)
Without a very careful assessment of the full range of motion, speed of motion and motion activity of the vocal folds during a variety of voice and non-voice tasks, an erroneous diagnosis of vocal fold paresis can be given to individuals who actually have vocal fold scarring (and vice versa).
Vocal Fold Scarring Often Occurs With Other Lesions
During the evaluation of vocal fold scarring, investigation of other possible associated lesions, such as vocal fold nodules, polyps, or cysts, is also necessary. (For more information, see Vocal Fold Lesions..)
- Vocal fold lesions must be investigated by both laryngoscopy and stroboscopy. (For more information, see Laryngoscopy/Stroboscopy.)
- Determining whether vocal fold lesions accompany vocal fold scarring is important since the treatment plan is different if is a combined problem exists.
- Vocal fold lesions may mask vocal fold scarring. Sometimes, because of the presence of large lesions of the vocal folds, scar tissue cannot be fully assessed or appreciated on stroboscopy and is not observed until microlaryngoscopy is performed under general anesthesia.
![]() Advisory Note
Advisory Note
Patient education material presented here does not substitute for medical consultation or examination, nor is this material intended to provide advice on the medical treatment appropriate to any specific circumstances.
All use of this site indicates acceptance of our Terms of Service.
Copyright © 2000-2006 Voice Foundation. All rights reserved.